Ambriel vs Assured
Side-by-side comparison to help you choose the right AI tool.
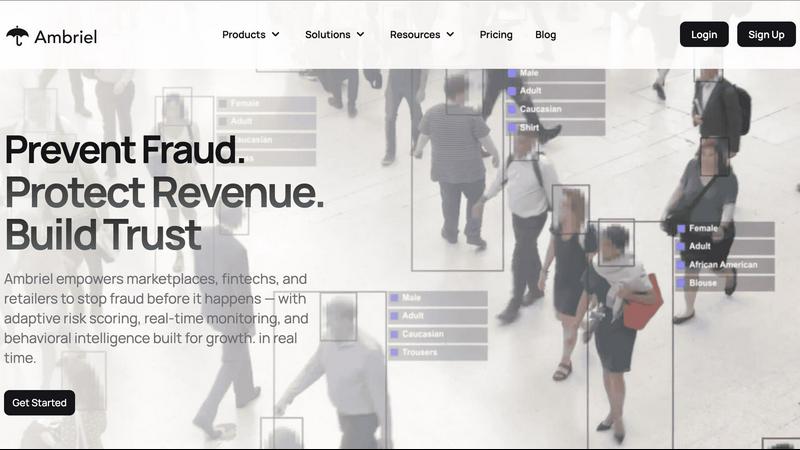
Trusted by innovators, Ambriel stops fraud in real time to protect your revenue and build trust.
Last updated: March 1, 2026
Assured
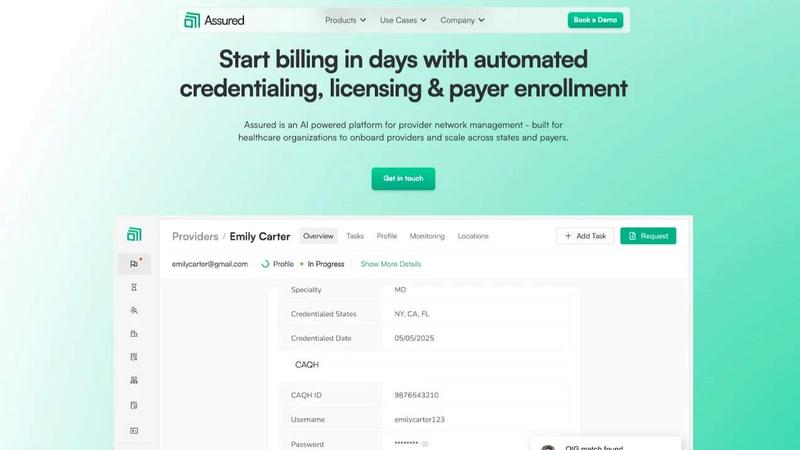
Assured uses AI to automate provider credentialing and enrollment so healthcare companies can start billing in days, not months.
Visual Comparison
Ambriel
Assured
Overview
About Ambriel
In the digital arena, where a single fraud attack can wipe out revenue and shatter hard-earned trust in an instant, Ambriel has emerged as the non-negotiable shield for growth-focused businesses. This isn't just another fraud tool; it's the intelligence platform that leading fintechs, marketplaces, and iGaming giants trust to operate fearlessly at scale. Ambriel provides the ultimate security blanket through a powerful, unified ecosystem that seamlessly blends behavioral analytics, cutting-edge device intelligence, automated sanctions screening, and real-time AI risk scoring. The viral appeal? Its uncanny ability to pinpoint and prevent sophisticated, revenue-draining fraud like synthetic identity creation, multi-accounting, and money laundering in real-time, all while ensuring a flawless, frictionless journey for your legitimate customers. Designed for innovators, Ambriel empowers you to protect your bottom line, ensure seamless compliance with global regulations, and build unshakable user trust. Join the thousands of companies that have made Ambriel their secret weapon for secure scaling, turning fraud prevention from a cost center into a competitive advantage.
About Assured
Assured is an AI-powered provider network management platform built to help healthcare organizations scale efficiently and stop losing revenue to administrative delays. It automates the complex, manual processes of credentialing, licensing, payer enrollment, and ongoing network monitoring. Designed for provider groups, health systems, payers, and digital health companies, Assured tackles the core problem of disconnected data and slow, error-prone manual work. Its core value proposition is dramatic speed and accuracy: get providers credentialed in 48 hours instead of 60+ days, achieve 95% first-pass approval rates for payer enrollments, and detect sanctions 22 days earlier than manual methods. As an NCQA-certified Credentials Verification Organization (CVO), Assured leverages AI to verify credentials across 2,000+ primary sources in parallel, auto-generate applications, and submit directly to payer portals. This means faster provider onboarding, quicker revenue generation, and complete peace of mind with real-time data monitoring, all from a single, centralized platform.
